How Long Does TMS Therapy Take to Work?
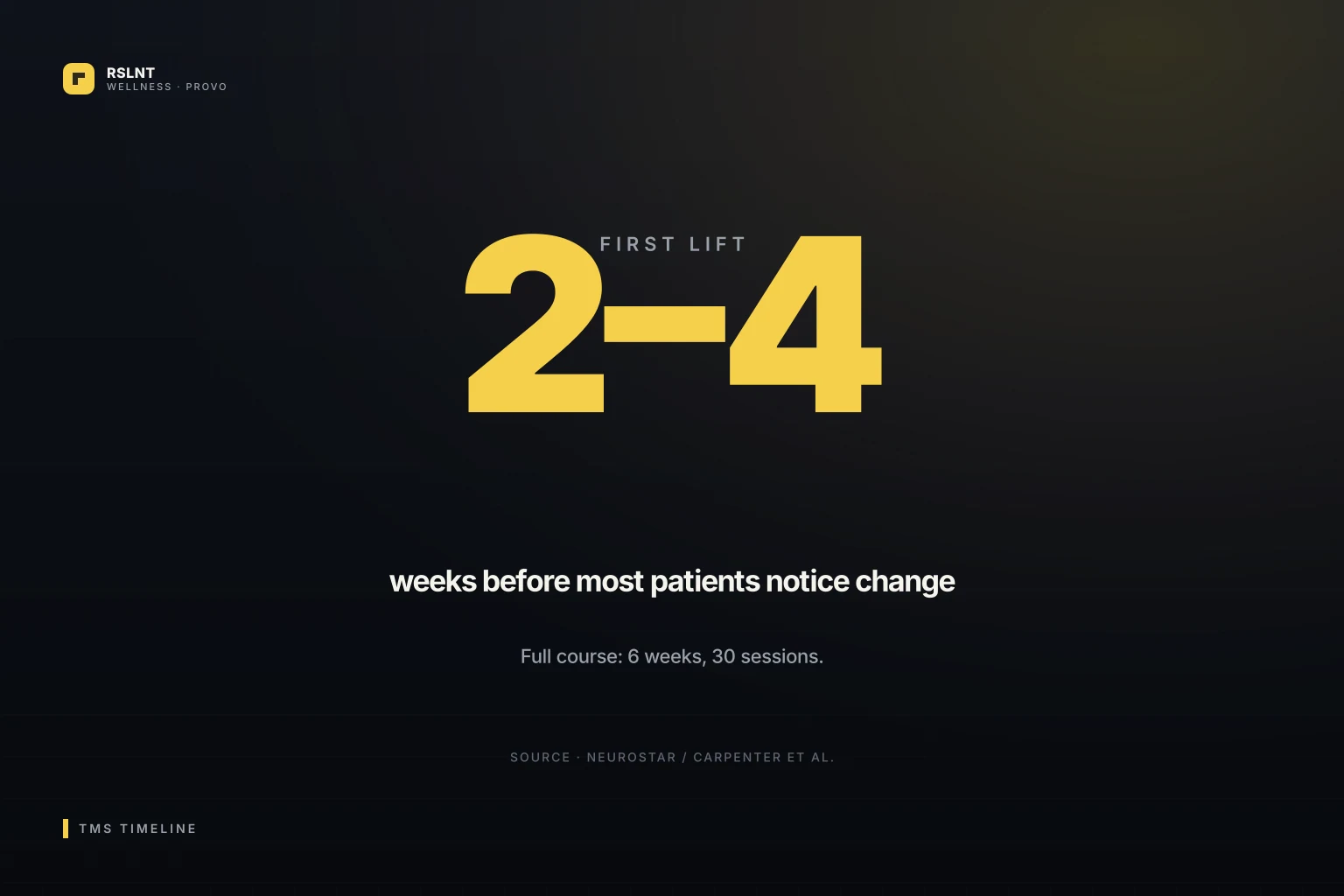
Table of contents
You've already given so many treatments time. The medication that took six weeks to settle in. The therapist you finally clicked with after the first three didn't fit. Now somebody is saying TMS, and your first thought is reasonable. How long until I know if this one works?
Fair question. You deserve a straight answer.
Most people start to feel a small shift between week two and week three of TMS therapy. The bigger lift usually shows up between weeks three and five. A full course runs about six weeks, with sessions five days a week at first, and most patients leave with a meaningful drop in their depression scores. Some feel it sooner. Some take a little longer. The brain responds on its own clock.
What the first week actually feels like
Week one is mostly about getting comfortable. The first session is the longest, around 45 minutes for the depression protocol, because we map your motor threshold, which tells us exactly how much energy your brain needs.
You'll feel a tapping on the side of your head. Not pain, more like a woodpecker on a hard hat. The first few sessions can be slightly uncomfortable while your scalp gets used to it. By day three or four, most patients describe it as boring.
You probably won't feel different yet. That's normal. Your brain is being introduced to something new. It hasn't had time to respond.
When the lift usually starts
Week two and three is where things get interesting. Patients describe it the same way over and over. Something is lighter. I don't know what.
The first sign is rarely a mood change. It's usually a sleep change. People fall asleep easier. They wake up less. The fog around mornings starts to thin.
Then the smaller things show up. You laugh at a podcast in the car. You text somebody back you've been avoiding. You eat lunch and actually taste it.
This is your dorsolateral prefrontal cortex coming back online. The part of your brain that handles motivation and emotional regulation has been undergunned for a long time. TMS is reminding it how to fire.
Why six weeks, not two
You'll see clinics online quoting different timelines. Three weeks. Five days. Some are real protocols. Some are aggressive marketing. The standard course cleared by the FDA for major depressive disorder is six weeks of daily sessions, Monday through Friday, then a two-week taper.
There's a reason for that. The brain doesn't change in three days. Neuroplasticity, the way neurons reshape their connections, takes repetition. Each session lays down a tiny piece of new wiring. Six weeks gives the brain enough reps to make the change stick.
When patients try to cut the course short because they're feeling better, the gains often slip back. We always recommend finishing.
What counts as a real response
The clinical word is response. If your depression score on the standard tool, the PHQ-9, drops by 50 percent or more, you've responded. If it drops to a level that says you're no longer clinically depressed, you've remitted.
Different studies show different numbers, but the broad picture is consistent. Around 60 to 65 percent of patients respond to TMS. Around 30 to 40 percent fully remit. These numbers are higher than what you see for someone trying their third or fourth medication after the first two failed.
Real-world response often looks like this:
- You can think about your future without dread sitting on your chest
- The cycle of bad sleep stops feeding the bad days
- You enjoy something specific again. A song. A plate of food. A walk.
- Therapy starts working better because you have enough fuel to actually use it
That last one is underrated. TMS doesn't replace therapy. It clears the static so the therapy can land.
When TMS doesn't move on schedule
Sometimes you hit week four and you don't feel much yet. That doesn't mean it isn't working. About 20 percent of responders are late responders. They get most of the lift in week five or six, or even in the maintenance phase.
If you're in week six and there's been no movement at all, we have other moves. We can extend the course, change the target site on the brain, or pivot back to a medication conversation. We don't pretend a treatment worked when it didn't.
How we actually treat this at RSLNT
At RSLNT Wellness, we run TMS the way the research says to run it. Five days a week for four weeks, then a two-week taper. We track your response with weekly PHQ-9 scores, not vibes.
Counseling alongside TMS. We pair TMS with talk therapy whenever possible. Patients who do both move further than patients who do TMS alone. Cognitive behavioral therapy or acceptance and commitment therapy works especially well during the lift.
Medication management. If you're already on an SSRI like sertraline or escitalopram, we don't take you off it during TMS unless there's a reason. Many patients keep their medication, and we adjust or taper later as the brain stabilizes.
TMS therapy. Sessions are about 19 minutes once we're past the first week. You can drive yourself to and from the appointment. No anesthesia, no needles, no recovery time. Patients often go straight back to work or school.
Frequently asked questions
Can I miss a session?
You can, and most people do at some point. Missing one or two sessions doesn't break the protocol. Missing five or six in a row can. We rebook missed sessions on the same week when possible.
Do I have to stop my medication during TMS?
No. Most patients stay on their current medication throughout the course. Stopping antidepressants suddenly is its own risk. We make changes carefully and slowly once the TMS has had time to take.
How long do TMS results last?
For many patients, the lift holds for a year or more, especially with periodic maintenance sessions. Some patients need a second full course later. The pattern depends on your history, your stress load, and whether the underlying causes have been addressed.
A six-week investment for a different brain
Six weeks is short compared to how long you've been carrying this. If you've been depressed for two years, that's roughly 100 weeks. You'd trade six for ninety four.
Schedule a free 15-minute consult. We'll look at your history, your medications, and what's still hard. If TMS is the right next step, we'll show you exactly what your six weeks would look like.
I'm not a therapist or a doctor. I'm someone who went from suicidal ideation, major depressive disorder, and crippling anxiety to clarity of mind. I feel like I got my life back. RSLNT Wellness is the place that helped me get there. If you're struggling, you don't have to figure this out alone.
Frequently Asked Questions
Can I miss a session?
Do I have to stop my medication during TMS?
How long do TMS results last?
Sources & Further Reading
Every clinical claim in this article is backed by a public, peer-reviewed, or government source. We do not cite anything we cannot link to.
- [1]Transcranial magnetic stimulation - Mayo ClinicMayo ClinicBacks: TMS is a noninvasive procedure that uses magnetic fields to stimulate nerve cells in the brain.
- [2]Transcranial magnetic stimulation - Mayo ClinicMayo ClinicBacks: TMS is generally used when other depression treatments haven't been effective.
- [3]510(k) Premarket NotificationU.S. Food and Drug Administration · 2008Backs: The NeuroStar TMS Therapy System was FDA-cleared in 2008 for major depressive disorder.
- [4]Transcranial magnetic stimulation - Mayo ClinicMayo ClinicBacks: TMS does not require anesthesia or sedation, and patients can return to usual activities afterward.
- [5]Depression - National Institute of Mental Health (NIMH)National Institute of Mental HealthBacks: Depression can affect sleep, energy, concentration, and daily functioning.
- [6]Cognitive Behavioral Therapy (CBT)American Psychological AssociationBacks: Cognitive behavioral therapy focuses on changing patterns of thoughts, feelings, and behaviors.
Ready to feel like yourself again?
Schedule a free consultation to see if TMS therapy is right for you.
Book Your Consultation